Eczema or psoriasis: understanding the key differences between these skin diseases
It is not uncommon to confuse eczema and psoriasis as these two skin conditions share symptoms such as red patches and itching. However, their origins, manifestations, and treatments are distinct. Clarifying these differences is essential for better skin care and daily management of the impact of these inflammatory diseases.
Location of lesions: a determining clue to differentiate eczema and psoriasis
The place where skin lesions appear represents a first differentiating sign. Atopic eczema mainly affects the flexural folds, especially the elbows, knees, wrists, and ankles. In infants, it is often accompanied by redness on the face, particularly the cheeks. You can deepen your understanding of these manifestations on specialized sites about atopic dermatitis.
In contrast, psoriasis rather targets areas subjected to friction or extension, such as the scalp, lower back, knees, elbows, and sometimes the nails, palms, and soles of the feet. However, it should be noted that some types like inverse psoriasis can affect the folds, which sometimes complicates the diagnosis.
Appearance of lesions: observe to better diagnose
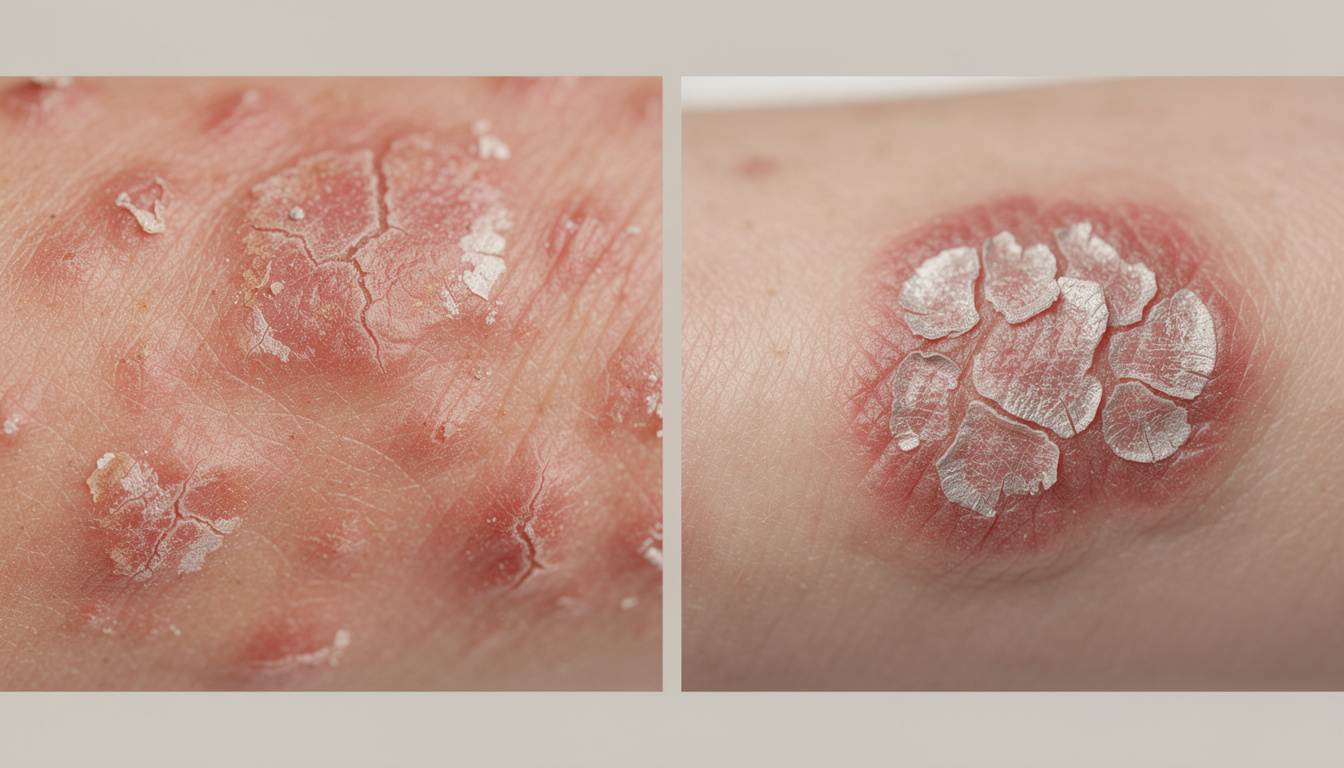
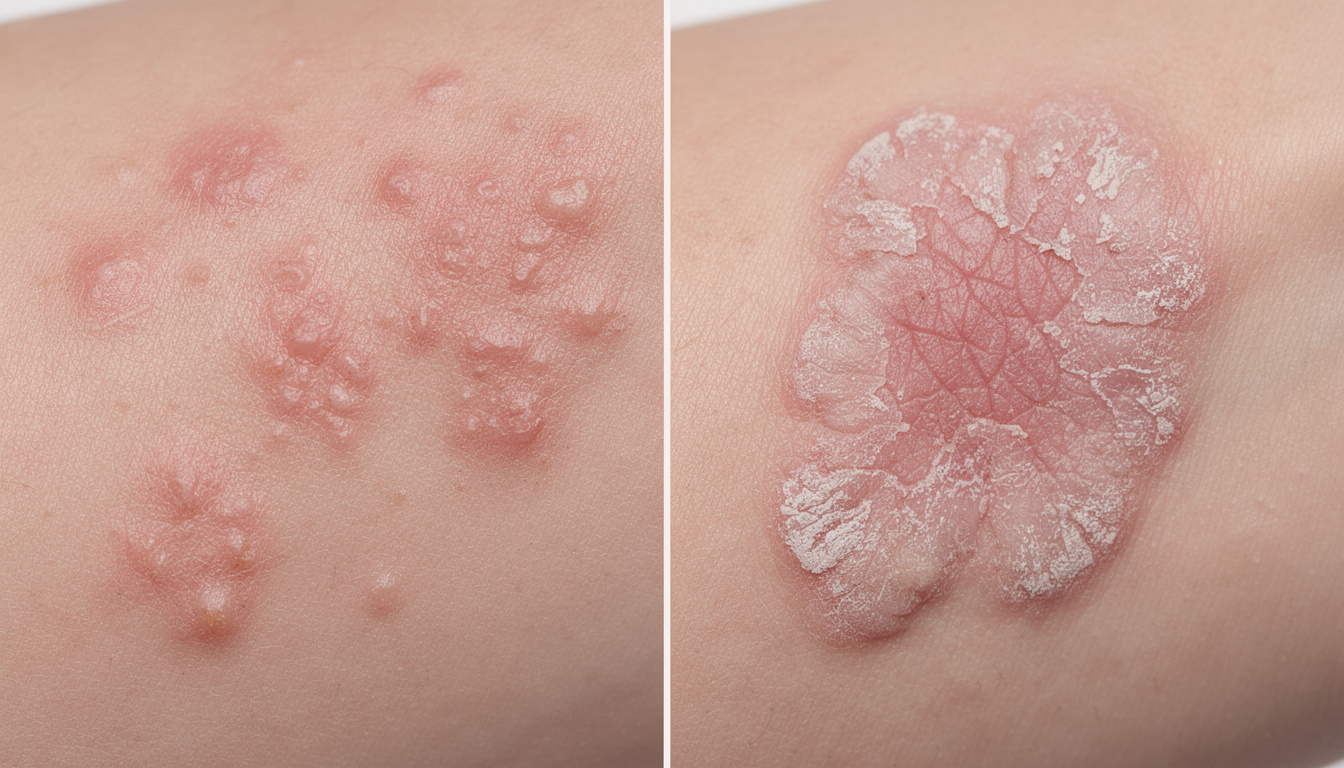
Taking a close look at skin plaques often helps to easily recognize the disorder. Lesions caused by eczema manifest as red inflammation, potentially accompanied by small vesicles that may ooze before forming crusts. The skin then becomes thickened and rough, sometimes tinged with brown.
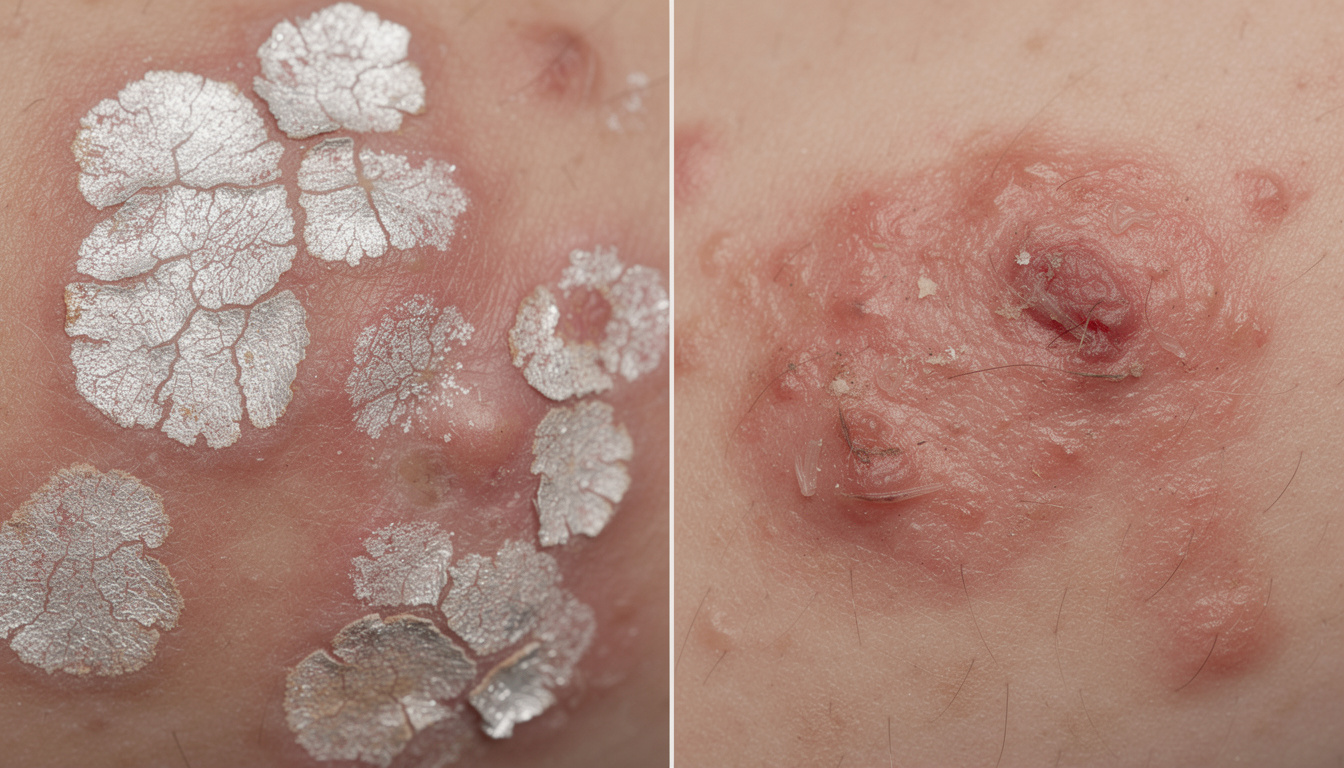
Psoriatic plaques are distinguished by their brighter redness and the presence of thick, white, and silvery scales that are easily detachable. Beneath, the skin appears red and shiny. Moreover, where eczema presents irregular and diffuse edges, psoriasis forms plaques with sharp borders, often geometric in shape.
Listen to your body: itching and associated symptoms for differentiation
Itching is present in both conditions, but its intensity differs significantly. Eczema causes violent, persistent scratching, often worse at night, strongly affecting sleep and quality of life. Psoriasis, sometimes without itching, may however cause sensations of tightness or burning with moderate scratching.
Another essential point: the triggering factors differ. Eczema is frequently exacerbated by allergens, emotional stress, climate changes, and exposure to certain fabrics. Conversely, psoriasis worsens with physical stress, infections, medications, or skin trauma.
Evolution over time: understanding the disease history to refine diagnosis
Atopic eczema usually appears from early childhood, with flare-ups interrupted by calm periods, tending to fade during adolescence or early adulthood. By contrast, psoriasis can appear at any age, with frequent peaks between 20-30 years and 50-60 years, evolving chronically with recurrent flare-ups without complete disappearance.
Response to treatments is also an important indicator: eczema is often well relieved by emollients and mild topical corticosteroids, whereas psoriasis frequently requires more targeted care, including potent dermocorticosteroids, vitamin derivatives, and sometimes systemic treatments.
When to consult a specialist and how to manage these conditions daily?
In the face of lesion extension, resistance to standard treatments, or the appearance of infection signs, it is crucial to consult a dermatologist. Only a professional can confirm the diagnosis, possibly with the help of additional tests, and guide you in setting up an appropriate protocol.
Here are some common tips to soothe your skin daily:
- Moisturize regularly your skin with suitable products to prevent dryness and limit flare-ups.
- Avoid temperature extremes that promote skin inflammation.
- Engage in relaxing activities to reduce stress, an aggravating factor of flare-ups.
- Choose soft textiles and avoid irritating products.
- Carefully monitor your plaques and note changes to better inform your doctor.
To better understand the complexity of skin diseases such as atopic eczema, many tools and associations are at your disposal.